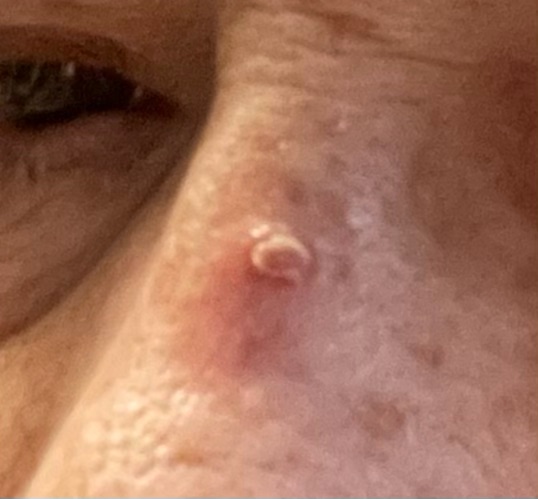
After I posted Just Nosing Around, I joined a Facebook group for Skin Cancer Warriors. I was amazed how supportive they are. I never had any support with Cushing’s or Kidney Cancer pre-op, so it was really nice to be on the receiving end for once.
From that FB group, I learned that May is Skin Cancer Awareness Month and there is a fundraising page (of course) so I actually decided to give it a try. I figure at least it will be another tshirt. LOL This is my page, if anyone is interested: Skin Cancer: Take a Hike!
Sunday, April 25, 2021. I’d been reading that handout I posted (below) and it’s made me start looking around for shirts that button, rather than pull over the head. I mostly have tshirts and some of those necks are pretty tight. I think I’m ok for at least tomorrow and the next few days.
Also, in preparation, I downloaded some books for my Kindle and started a few coloring images in Happy Color so that I wouldn’t have to use WiFi to download there.
Also, I remembered that I should stress dose tomorrow! I started packing my bag to include Tylenol and I’ll add extra cortisol, a bottle of ice water and my iPad tomorrow.
So, Monday, April 26, 2021 I had my Mohs Surgery.
I remembered to take my extra cortisone! We got there 30 minutes early, which worked in our favor – for once.
Tom could go in with me while I had my surgery and I stayed in room the whole time. The nurse came in and we went over basic questions. The surgeon came in and recognized where the location was – he could see it over the top of my mask. He explained what he’d do and asked if there were any questions, then used a marker to make a circle around the cancer.
He injected the pain killer. I started when it first went in but then it was ok. He asked if I could feel anything. I said no so he continued.
They bandaged everything, cauterized the blood vessels and took the cancer off to the lab.
When they came back, the surgeon said that the cancer was gone. He used dissolvable stitches and a skin graft. I could see quite a bit of blood during this. He did more cautery and the nurse put on lots of bandages which I had to keep on for 24 hours. Because of the skin graft, he called in antibiotics.

Tom drove home – it was hard for me to see over bandages. About 1 pm I took 3 Tylenol. I took first antibiotic about 2 pm – Doxycycline Hyclate 100 mg. I take those twice a day for 10 days because of the skin graft.
Then, I fell asleep and woke up about 8:30PM and had some dinner. 3 more Tylenol and another antibiotic.
I slept ok overnight and woke up about 5:30 am with pressure from the bandages on my face. I tried to sleep for about another hour, then just got up. No real pain just a dull ache. If I touch my nose, it does hurt…so – don’t touch!
Tuesday, April 27, 2021, I kept my video off for my work Zoom meeting so no one would see all those bandages. I skipped an in-person afternoon meeting but about 4:00 pm I got to change the bandages so I could see what I’m dealing with:

Right at the bridge of my nose it’s a little bit swollen and it’s uncomfortable to wear my glasses. I had a handbell rehearsal Tuesday night that I also skipped.
Wednesday is normally one of the three days a week I do water exercise but I can’t get this thing wet so I stayed home and did a little work. I didn’t take the antibiotics with food, just with coffee, and that really upset my stomach. I ended up cancelling my piano students for the afternoon. They had all asked last week about the biopsy bandage – I wasn’t sure how I would explain this one to a first grader. My stomach was still upset from the antibiotic anyway.
I had bought new bandages on amazon that were supposed to be latex-free. I think they skirted around that claim somehow because as soon as I tried them, my nose was itchy. At first, I thought maybe my nose was healing but I ripped off the bandage and went back to the old plastic ones that made my nose red. The itching stopped but after that, I had a lot of trouble sleeping and finally just got up about 3:00 am.
Other healing pictures:
April 30, 2021:

May 2, 2021

Update May 7, 2021. Big Day – I finally went back to water exercise after nearly 2 weeks off and it felt so good to be back, to be normal. Besides that, I ran into my son’s elementary school music teacher (I had also been her piano accompanist) and we chatted about how things were going.
I also went (nervously!) to my main dermatologist for a full body scan and no other skin cancer was found.
May 8, 2021, Healing better than I thought it would.

May 24, I go back to my surgeon where I will (I hope!) get more good news. Assuming it’s good news, this post is done.
If not, there will be yet another update.
It seems like my nose is always at the forefront of my medical issues. Cushing’s disease? Let’s do a whole surgery through her nose.
Allergies? Let’s clog up her nose so she can’t breathe.
Kidney cancer? Let’s stick tubes up her nose so she can breathe.
None of that stuff did her in, so let’s try playing with the outside this time.
I hadn’t thought much about my nose lately unless I was adjusting a mask over it for COVID. Luckily, I was never tested for COVID because that would have been a swab…up my nose.
In January 2021, I was just keeping my nose out of other people’s business when I noticed weird stuff on my nose. I made the obligatory doctor appointment. He thought that part of my issue was allergies to paper masks and gave me cream – guess what!?!? – Kenalog, a steroid cream form of the stuff they inject into my knee. Part of the description for that reads “Do not use it on the face, groin, or underarms unless directed to do so by your doctor.” I was directed by my doctor so I guess it was ok but I sure hate using additional steroids.
In the middle of the nose-redness to be fixed by Kenalog was a really weird thing. The doctor thought it would be useful to use liquid nitrogen on it and I figured that was relatively easy so I went for it.
So, he sprayed the nitrogen on and said to use the Kenalog twice a day – the thing should fall off in a couple weeks. A couple weeks spread out to about 5 and it fell into my mask a day or so after I had a dream about it falling into the swimming pool and infecting everyone there. Fortunately, my dream didn’t come true!
Unfortunately, when it fell off, it left a hard red bump which stuck around and started looking weird again.
So, February 22, I called the doctor again and made an appointment for March 10. He said he could do the nitrogen thing again and go a bit deeper. I thought, maybe no. Let’s move on to the professionals. So, I got a referral to a dermatologist on April 16.
Even with my mask on, the dermatologist could see the top peeking out of my mask and proclaimed Squamous Cell Carcinoma! She did do a biopsy, so I had a few days of hope. I thought the biopsy would be a smaller amount, though.
So, I put Aquaphor and a bandage on my nose twice a day…and my nose got red under the bandaid. Allergy to the adhesive? I know I’m allergic to latex, so we have plastic bandaids. Whatever.
April 21 I got the official results. The dermatologist was right the first time. Monday, April 26 I will have Mohs surgery.
Of course, I set out to watch this surgery on YouTube.
I downloaded the handbook mentioned at the above video. Find it at https://www.dartmouth-hitchcock.org/sites/default/files/2020-12/mohs-handbook.pdf.
Because I always “own” all my diseases, I bought a t-shirt which I will wear proudly. Of course, it has a butterfly and the words: “They whispered to her – you cannot withstand the storm. She whispered back – I am the storm.” and Squamous Cell Carcinoma Awareness.

I have so many t-shirts – not just for places but for causes, diseases, work, piano teaching… I hope this is the last non-fun one I get!
I am not anticipating any changes in this over the weekend so the next post will be sometime next week, after the surgery.
Thanks for any prayers, good wishes, whatever!